Your Achilles tendon is the strong fibrous band of tissue that connects your calf muscles to your heel. The tendon is named after “Achilles” who was a powerful, yet vulnerable warrior in Greek mythology. Likewise, our Achilles tendon, being the largest and strongest tendon in the body, is susceptible to injury from the high demands placed on it (running can generate forces over 12 times your body weight on the Achilles tendon).
The tendon may be strained or even ruptured from excessive stretch or forceful contraction of the calf muscles. More commonly, the tendon is repeatedly overloaded and suffers tiny “micro-tears.” Damage usually occurs either directly behind the heel or near the weakest area of the tendon- one to two inches above the heel.
Achilles tendon injuries affect between 250,000 and 1 million people per year. Most are middle-aged males, between the age of 30 and 50. Interestingly, Achilles tendon injuries occur more frequently on the left side. If you have suffered a prior Achilles tendon injury, you are at greater risk of injuring the opposite side. Two-thirds of all Achilles injuries involve athletes. Runners are up to 10 times more likely to suffer Achilles tendon problems. You may be at increased risk if the arch of your foot is too high or too flat.
Symptoms may begin abruptly following a strain but more commonly develop slowly from repeated irritation. Morning pain and stiffness are common. Your symptoms will likely increase with activity, especially walking or running. You may notice pain when you rise on your toes. Walking downstairs stretches the tendon and usually increases symptoms. Some patients notice that the irritated area becomes firmly swollen. Ongoing irritation to the spot on your heel where the tendon inserts can cause a painfully elevated “pump bump.”
Research has shown that conservative care, like the type provided in our office, can produce “excellent results” in over 85% of patients.
Initially, you may need to limit or stop activities that cause pain. Runners may need to switch to swimming or cycling for a short period of time. Be sure to introduce new activities slowly and avoid increasing your activity by more than 10% per week. Runners should begin on a smooth, shock-absorbent surface and start at a low intensity – first increasing distance, then pace. Avoid training on hard or unlevel surfaces like hills. Make sure you warm up properly and avoid over-training. Avoid wearing compression socks, high heels, or shoes with an excessively rigid heel tab. One of the most important and effective treatments for Achilles tendinopathy is performing “heel drop exercises” as outlined below.
THINGS YOU CAN DO TO HELP YOURSELF
Your everyday activities, habits, and postures can have a dramatic impact on your body. The following advice will help you minimize stress while improving your comfort and health:
Footwear
Improperly supported feet can affect the alignment of all of the structures above. To improve your overall comfort:
– Choose shoes with good arch support.
– Avoid going barefoot or wearing shoes that lack support (i.e. flip-flops). The following brands of sandals provide better than average arch support: Naot, Fit Flops, Orthoheels, Abeo, Vionic, and Yellow Box.
– Avoid high-heeled shoes or boots (keep heels to a maximum of 1½ inches, especially if you are going to be doing a lot of walking).
– “Cross-trainer” athletic shoes tend to provide the best all-around support and shock absorption for daily activities.
– Patients with fallen arches should consider adding arch supports or orthotics.
– Repair or replace shoes with worn soles or heels.
Running Shoes
Running shoes need to be replaced every 250 miles or ~400 Km. There are three basic options:
– Motion Control Shoes – Designed for people with low or no arches, these shoes are for runners who strike the ground on the outer edge of their feet. Avoid overly stiff shoes as these decrease your perception of the ground strike and lead to new injuries.
– Stability or Neutral Shoes – Designed for people with normal or average arches and running mechanics. The shoe contains some cushioning to absorb shock and prevent injuries and some rigidity to avoid pronation.
– Cushioned Shoes – Designed for people with high arched feet. Their footprint will typically leave a thin band along the foot’s edge. As they run weight is distributed from heel strike to the outer edge of the foot and small toes that bear the brunt of “lift-off.” This shoe is more flexible and absorbs the shock created by the lack of rotation (under-pronation) created by their running style.
Home Exercises:
Standing Gastroc Stretch
Perform 1 set of 3 contract/relax cycles, 2 times per day.
Stand facing a wall with your hands on the wall at head level. Your affected leg to be stretched should be back and straight with your heel on the floor. Your unaffected leg may be bent in front of you for support. While keeping your back straight, lean forward until you feel a stretch in your calf. Against the resistance of the floor, attempt to push the toes of your trailing foot into the floor for seven seconds. Do not lift your heel off of the floor. Relax and lean further forward to increase the stretch. “Lock-in” to this new position and repeat three contract/relax cycles on each side twice per day or as directed.
Standing Soleus Stretch
Perform 1 set of 3 contract/relax cycles, 2 times per day.
Stand facing the wall with the ball of your affected foot on the wall, heels on the ground with your other leg behind you for stability. As an alternative to placing your foot on the wall, you may step on a 2-4 inch block or book on the floor in front of the wall. Place your hands on the wall for additional stability. Bend your forward knee while lowering your body toward the wall until you feel a strong stretch in your calf. Against the resistance of the wall/ block, attempt to flex the front of your foot toward the floor. Hold this contraction for seven seconds. Relax and stretch further. “Lock-in” to this new position and repeat three contract/relax cycles on each side twice per day or as directed.
Eccentric Achilles Strengthening
Perform 6 sets of 15 reps, 2 times per day.
Notes: 3 with straight knee and 3 with slightly bent knee
Begin standing up on your toes with the affected foot on the edge of a step. Do not place weight on your good leg, but you may use it for stability. Slowly lower your affected heel, at a count of 4 seconds, until you reach a fully stretched position and can drop no further. Use your good leg to return to your toes. Perform as directed. Moderate pain during this exercise is acceptable but if the pain is excessive, you should assist downward motion with the non-injured leg.
Evidenced-based rehabilitation treatment we offer
Here is a brief description of the treatments we may use to help manage your problem.
Therapy Modalities
We may apply electrotherapy modalities that produce light electrical pulses transmitted through electrodes placed over your specific sites of concern. These comfortable modalities work to decrease your pain, limit inflammation and ease muscle spasms. Hot or cold packs are often used in conjunction, to enhance the effect of these modalities.
Another available option is therapeutic ultrasound. Ultrasound pushes sound vibrations into tissues. When these vibrations reach your deep tissues, heat develops, and unwanted waste products are dispersed.
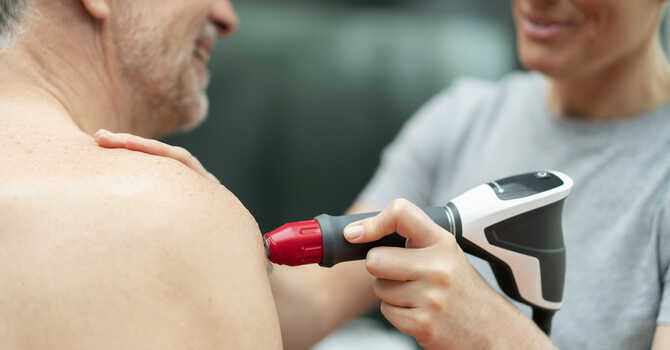
Shockwave Therapy is another treatment option that is successful in treating Achilles tendonitis. Shockwave Therapy is a non-invasive therapeutic device that works by delivering acoustic waves to the site of injury. The use of shockwave therapy for Achilles tendinopathy is well supported by high-quality research studies.
Myofascial Release
Overworked muscles often become tight and develop knots or “trigger points”. Chronic tightness produces inflammation and swelling that ultimately leads to the formation of “adhesions” between tissues. Your provider will apply pressure with their hands, or with specialized tools, in order to release muscle tightness and soft-tissue adhesions. This will help to improve your circulation, relieve pain and restore flexibility.
Therapeutic Exercise
Muscle tightness or weakness causes discomfort and alters normal joint function, leading to additional problems. Your chiropractor or physiotherapist will target tight or weak muscles with specific therapeutic stretching and strengthening to help increase tissue flexibility, build strength, and ease the pain. Healthy, strong, and flexible muscles may help prevent re-injury.
Foot Evaluation
Fallen arches and faulty foot mechanics are common problems that can perpetuate your condition. Our office will carefully evaluate your feet and consider the need for a change in shoe style, arch supports, or even custom orthotics.
Contact Heal Physiotherapy & Chiropractic North York today to learn more!